
Patient Identification
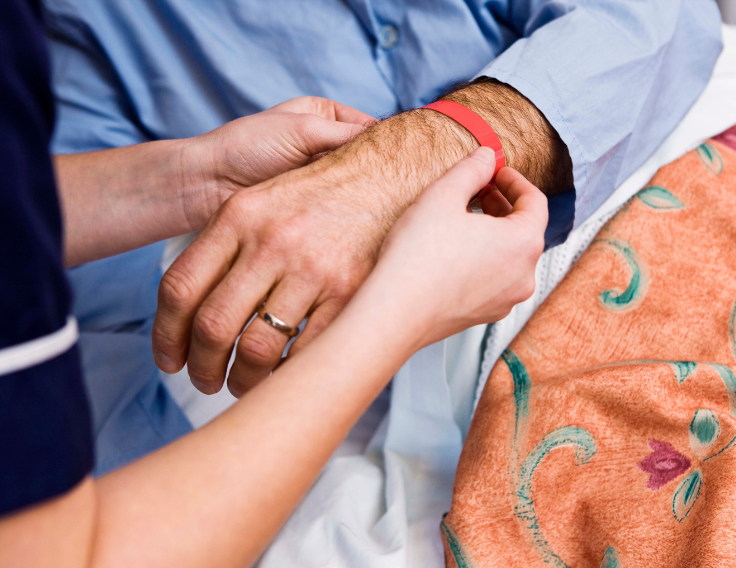
Patient identification links a patient’s medical record across various health systems [1]. This provides a complete view of a patient’s record which can be useful in preventing adverse health effects. Oftentimes, patient identification is done by linking different demographic information such as date of birth, name, and address [1]. Currently, most hospitals implement armbands as a method of keeping track of patient identification. They are especially beneficial in times of emergency and allow doctors to keep track of what medicine has already been provided and the different treatment options the patient has completed during their stay [2]. This helps to improve patient safety and can prevent patients from receiving medicine or treatment that could cause adverse health effects. However, the current system isn’t free from error, and health IT tools need to create better solutions to address patient errors and interoperability issues.

Current Areas Where Patient Identification Fails
There are various issues that may rise with the wrong patient identification. First, patients may be linked to different health record data and receive improper care [3]. Another issue is during stressful times of an emergency room visit, the EHR data may not show up correctly for a patient [3]. This means that the doctor will either be unable to find the patient’s health record, or they may select the wrong record to go with. Furthermore, it may take too long to find a patient’s health record from the EHR system, especially in high-pressure situations like during an emergency visit. Human errors can also result from nurses or doctors incorrectly scanning patient barcodes, or not scanning them after administering treatment. Another issue is duplicate medical records, which happen when the doctor is unable to find the original health record [3]. This can lead to fragmented and less effective treatment.

All of these issues are concerning because they reduce patient safety. Diagnostics and medical errors are one of the most common errors that patients may face [4]. Another error is during surgery when the wrong surgery is provided to a patient [4]. Furthermore, patients must consent to the treatment that they receive, and sometimes do-not-resuscitate orders may not be followed in stressful situations or due to mix-ups with patient identification. These areas are a concern for patient safety and can affect the quality of life of the patient. Furthermore, almost half of the adverse effects can be prevented, which means that newer technology must be put into place to better identify patients [5]. Better patient identification technology is needed to keep patients’ health records updated with the most current information and to correctly track patients during their visits.
Implementing AI Tools to Innovate Patient Identification
AI is an effective method to link patients to their health records faster and more accurately. It can also be used to correctly identify the patient and aid the doctor with diagnosing. One useful benefit of patient identification is to have a database for treating rare conditions. AI can use face recognition from patient photos to identify rare conditions in patients [6]. Moreover, AI can predict which patients may be more likely to have a diagnosis for certain illnesses. This is useful for pharmaceutical companies who may want to have a list of physicians treating patients with newer drugs that could provide an effective treatment option [6]. AI also helps to link patients to new clinical trials and can calculate success depending on whether the patient meets the criteria for the study [6].
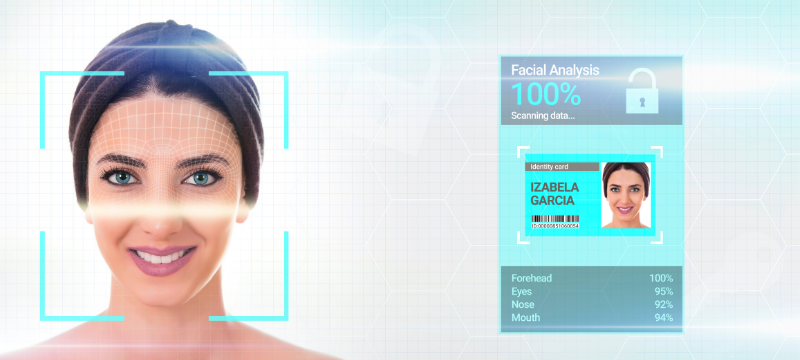
Overall, AI is a useful tool for taking patient identification beyond a hospital visit. It can be used to track treatment options for patients, make diagnostic suggestions, and suggest patients for newer treatment options.
Health IT Tools that Improve Patient Identification
Health IT tools can promote patient safety measures by optimizing fast and reliable patient identification. One method is by establishing a two-factor authentication system that asks patients for additional data such as their address or other personal data to prevent mismatching [7]. Another method is to promote automated tools that help reduce errors. This can be done with barcodes and biometrics that keep human error out of the identification process [7]. Additionally, EHR systems can use photo identification to assist in verifying that the correct patient receives treatment [7].
All of these solutions go back to human-centered design, which means that systems are created with the intent of meeting functional requirements [8]. Health IT developers need to create solutions and systems that are useful to patients and promote interoperability. This means that the system must be easy to follow and track with an appropriate user interface that promotes correct patient identification across various systems and reduces human error. An important tool in promoting human-centered design is implementing a clinical decision support (CDS) system [8]. CDS provides a user interface that allows doctors and patients to receive alerts and remote monitoring [8]. Overall, CDS systems make it easier for doctors to store, track, and manage patient data and can promote patient safety. Overall, health IT technology is crucial to improving patient identification and can lead to better health for patients.
HITS
HITS provides healthcare management services & works with doctors to develop health informatics tools that promote safe and secure care. We take pride in our services and settle for nothing other than 100% quality solutions for our clients. Having the right team assist with data sharing is crucial to encouraging collaborative and secure care. If you’re looking for the right team, HITS is it! You can reach out to us directly at info@healthitsol.com. Check out this link if you’re interested in having a 15-minute consultation with us: https://bit.ly/3RLsRXR.
References
- https://www.healthit.gov/topic/interoperability/standards-and-technology/patient-identity-and-patient-record-matching
- https://www.assetinfinity.com/blog/patient-id-wristband-in-healthcare-industry
- https://www.rightpatient.com/blog/common-reasons-for-patient-identification-errors-in-hospitals/
- https://www.rosenbaumnylaw.com/blog/2021/07/the-most-common-medical-errors/
- https://healthinformationtechnologysolutions.com/patient-safety-advances-with-health-it/
- https://eularis.com/can-you-find-your-patients-using-ai-for-faster-patient-identification-and-treatment/
- https://www.m2sys.com/blog/guest-blog-posts/patient-identification-why-its-important-and-how-best-ways-to-implement-it/
- https://healthinformationtechnologysolutions.com/getting-back-to-the-basics-of-human-centered-design/